Mild swelling and discomfort are completely normal bodily responses during the first few days after oral surgery. However, the line between normal healing and complications can often be confusing for many patients. So, what are the signs of infection after tooth extraction? Let Shark Dental Clinic guide you through the detailed information in the article below!
Common signs of infection after tooth extraction
After a tooth extraction, mild pain and slight swelling during the first few days are normal reactions. However, if these symptoms do not improve and instead worsen, they may indicate an infection that requires prompt treatment.
Warning sign 1: Persistent or worsening pain beyond day 3
Patients often ask, “how long does tooth extraction take to heal?” Typically, pain after an extraction peaks within the first 24 hours and gradually decreases. If you find that the pain does not diminish and becomes increasingly intense after 2-3 days, this is a common sign of infection. If the pain does not respond to standard pain relievers, it could indicate an infected socket or the development of a dry socket.

Warning sign 2: Abnormal swelling and redness spreading to the neck
Facial swelling is a natural response, but it usually subsides after 48 hours. If the swelling becomes firm, hot, red, and spreads to the neck or under the jaw, it could be a sign of infection. More critically, if the swelling leads to difficulty opening your mouth, swallowing, or breathing, you should see a dentist immediately.
Warning sign 3: Presence of pus, discharge, or foul taste
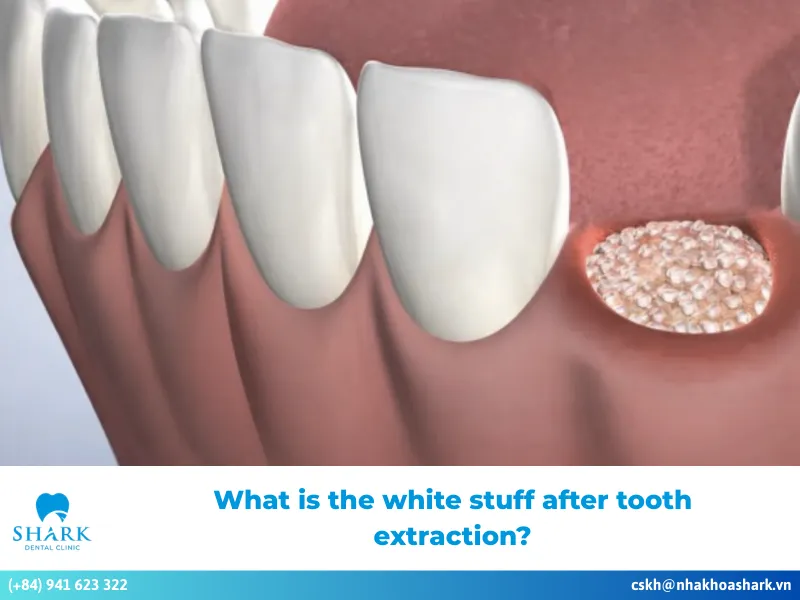
In contrast to normal pale pink plasma or the healthy white stuff after tooth extraction known as granulation tissue, infectious discharge is typically thick and yellow or white. This may be accompanied by a strong, foul odor and a persistent bitter or unpleasant taste in the mouth, even after rinsing. This is clear evidence that bacteria are accumulating in the socket.
Warning sign 4: Systemic symptoms like fever and swollen lymph nodes
As an infection progresses, the body may react with an elevated temperature, resulting in fever or swollen lymph nodes in the neck or under the jaw. These symptoms indicate that the immune system is fighting bacteria, and you should visit your dentist or a medical facility for an examination as soon as possible.

What causes infection after tooth extraction?
Infection signs after tooth extraction can stem from various factors related to aftercare habits, overall health conditions, and the extraction procedure itself, including:
- Food debris retention: Trapped food particles can decompose and foster bacterial growth.
- Poor oral hygiene: Inadequate brushing and cleaning can allow bacteria to invade the wound.
- Unhealthy habits: Smoking and alcohol consumption can dislodge blood clots and weaken the oral mucosa.
- Weakened immune system: Elderly individuals, as well as those with diabetes or chronic illnesses, may have a reduced ability to fight infections.
- Large surgical wounds: Extracting difficult or impacted teeth often results in larger wounds more susceptible to bacterial invasion.
- Non-sterile extraction instruments: Cross-contamination can occur from dental tools that are not properly sterilized.
- Pre-existing infections: Bacteria may spread from other infected areas in the body to the newly extracted site.

Why wisdom teeth are more prone to infection?
Wisdom teeth, being the last to erupt and located at the back of the dental arch, have a higher risk of infection after extraction. This is due to several factors:
- Difficult-to-clean position: Wisdom teeth are hard to reach with a regular toothbrush, making them prone to food and plaque accumulation, which fosters bacterial growth.
- Impacted or partially erupted growth: Often, wisdom teeth grow under the gum or only partially emerge, increasing the likelihood of inflammation in the surrounding tissue.
- Complex extraction procedure: Removing wisdom teeth frequently requires incisions in the gum or deeper intervention in the jawbone, resulting in larger wounds that demand thorough care.
- Longer recovery time: Due to greater tissue trauma, sites of wisdom tooth extraction need more time to heal. During this recovery period, improper care significantly heightens the risk of infection.
How tooth extraction infections are treated
When signs of infection occur after a tooth extraction, it is essential to see a dentist promptly to manage inflammation and prevent serious complications. Treatment options may include:
- Medication: Dentists typically prescribe antibiotics to eliminate bacteria, along with pain relievers and anti-inflammatory medications at the appropriate dosage. An antiseptic mouthwash may also be recommended to disinfect and clean the affected area.
- Drainage of abscess: If an abscess develops, the dentist may perform an incision to drain the pus, preventing the spread of bacteria to healthy teeth and surrounding tissues.
- Deep socket cleaning: The dentist will remove any necrotic tissue and thoroughly clean out food debris or foreign materials left in the socket to eliminate the source of infection.
- Advanced medical intervention: In severe cases, where there is a risk of systemic spread, hospitalization may be necessary for high-dose intravenous antibiotics and close health monitoring.
How to reduce the risk of infection after tooth extraction
To minimize the risk of infection following a tooth extraction and promote safe healing, consider these five key principles:
- Choose a reputable dental clinic: Select clinics with stringent sterilization protocols to eliminate the risk of cross-infection right from the start. Finding a trusted provider for a tooth extraction in Ho Chi Minh City is a great first step.
- Follow prescribed medication instructions: Take antibiotics and pain relievers precisely as directed. Avoid stopping medication prematurely to prevent antibiotic resistance.
- Apply cold compresses to reduce swelling: Using ice packs on the outside of the cheek helps constrict blood vessels, alleviate pain, and diminish swelling effectively.
- Prioritize soft foods and adequate hydration: Drink plenty of water and consume soft, cool foods. It is best to avoid hard or overly hot foods that may irritate the extraction site.
- Maintain proper oral hygiene: Brush your teeth regularly with a soft-bristled toothbrush, being cautious to avoid direct contact with the extraction site. After 24 hours, you may gently rinse with a saline solution to help clean the area and reduce bacteria.
- Avoid smoking and alcohol: These substances can hinder healing and create an environment conducive for bacterial growth. It is advisable to abstain from both until the extraction site stabilizes.
When to call a dentist for post-extraction infection?
After a tooth extraction, mild soreness or slight swelling is typical. However, you should contact your dentist immediately if you experience any of the following signs of infection:
- Severe pain or pain that intensifies over time, particularly after 2 to 3 days instead of improving.
- Significant swelling, redness, or any spreading to the cheek, jaw, or neck area.
- The presence of pus or foul-smelling discharge, accompanied by an unpleasant taste in the mouth.
- Prolonged, uncontrolled bleeding.
- Fever, fatigue, or swollen lymph nodes under the jaw or in the neck.

The information shared by Shark Dental Clinic emphasizes that early recognition of signs of infection after tooth extraction allows for proactive measures before the situation escalates. A timely dental examination not only reduces the risk of complications but also ensures a safer and quicker recovery process.