In diagnosing and treating dental conditions related to the pulp and dental abscesses, X-ray imaging is considered an essential and highly important indication. This method allows the dentist to observe abnormal changes and formulate an effective treatment plan. So, what does an abscessed tooth infected root canal X-ray look like? Let’s explore the detailed answer in the article below!
What does an abscessed tooth infected root canal X-ray look like?
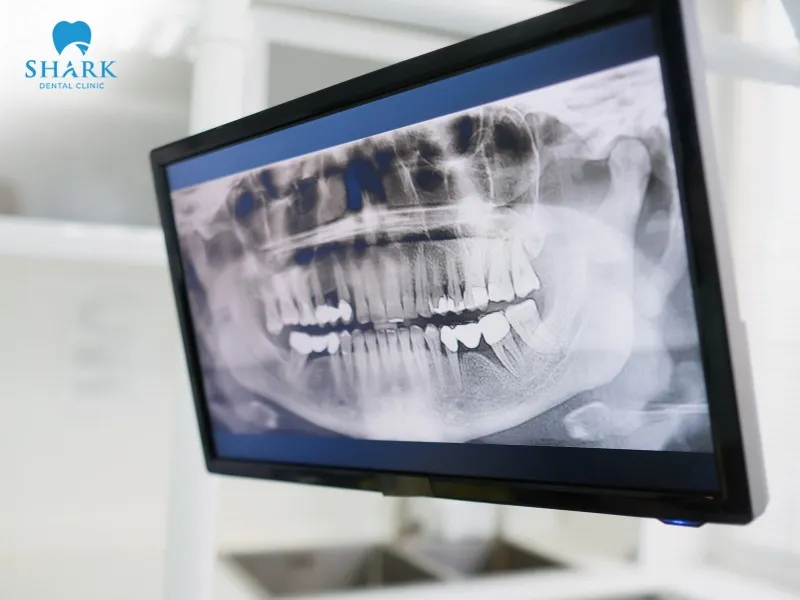
When a tooth is healthy, a dentist will see evenly colored margins on the X-ray film with moderate radiodensity. However, if an infection or dental abscess is present, the X-ray images of an abscessed tooth with an infected root canal will show several noticeable changes:
- When a tooth develops an abscess, the bone around the root tip becomes damaged. On the X-ray, this appears as a darker area compared to the surrounding healthy bone. This dark region may be oval or round, and the larger the dark patch, the more severe the abscess is. Dentists rely on this contrast when learning how to read a dental X-ray accurately.
- In healthy tooth structures, a thin line surrounds the root tip. However, when there is an infection or abscess, these margins become thicker or may appear faded. This is a warning sign that the area around the root tip is being destroyed by inflammation.
- In some cases, the dark area around the root tip appears perfectly round with a clear border, indicating that the abscess has existed for a long time. If the dark area spreads widely with an unclear margin, it may indicate a progressing infection with ongoing bone resorption.
- If the tooth has not undergone root canal treatment and the canal remains healthy, the X-ray will clearly show the root canal running from the crown down to the root tip. Conversely, if an infection is present, the canal may appear narrow or calcified, which can be observed on the X-ray film.
>>> See more: Can a dentist remove a root canal tooth?
What are the red flags for dental abscess?
A dental abscess or tooth infection is a serious condition that can adversely affect oral health and negatively impact daily quality of life. Early symptoms may begin with toothache or gum swelling, but over time, the pain can become severe and may be accompanied by a high fever.
Here are several key warning signs of a dental abscess that you should never ignore:
- Toothache: Initially, you may experience dull, intermittent tooth pain, often worse at night. Many people find that chewing or even lightly touching the tooth causes discomfort.
- Tooth sensitivity: As the abscess progresses, the tooth may become extremely sensitive. You might feel sharp pain or tingling when consuming very hot or very cold foods. This sensitivity indicates that the pulp or tissues around the root tip are inflamed.
- Swollen gums or face: A dental abscess can lead to swollen gums, cheeks, or painful swelling around the tooth root. As the abscess spreads, the area under the jaw—and even the eyes or lips—may feel tight, swollen, or uncomfortable.

- Presence of pus: When an abscess forms, pus pockets may develop in the soft tissue or within the tooth socket. Initially, these pockets are small, white, and soft. Over time, they may turn yellowish and develop a foul odor.
- Tooth discoloration: Another noticeable sign is tooth discoloration. This usually occurs when the pulp tissue inside the tooth becomes necrotic, causing breakdown products to seep into the porous tooth structure and darken the tooth.
- Fever and fatigue: If an abscess spreads widely and the infection becomes severe, the body may respond with fever, weakness, and fatigue. Many patients also worry about systemic effects and ask, “Can an infected root canal cause high blood pressure?” While an infection itself doesn’t cause chronic hypertension, the acute pain and stress of a severe dental abscess can lead to temporary spikes in blood pressure. Prolonged infection can lead to sepsis, which is extremely dangerous and requires immediate medical intervention.
- Swollen lymph nodes: During an abscess, the lymphatic system attempts to filter and eliminate the bacteria. As a result, the lymph nodes under the jaw and neck may become enlarged, firm, and movable.
- General discomfort: When you experience a dental abscess or infected pulp, your body may feel drained and generally unwell, as it expends significant energy fighting the infection.

If you notice any of the abnormalities or symptoms mentioned above, it is essential to inform your dentist immediately. Your dentist will perform an X-ray along with a clinical examination to assess the condition, provide the right advice, and offer timely treatment. While many patients ask about the Dental X-ray cost during their initial inquiry, this diagnostic step is vital for ensuring your safety and is a foundational part of high-quality comprehensive dental care services in Vietnam.
>>> See more: Can a root canal get infected?
How soon after a root canal can issues appear on X-rays?
After a root canal treatment, abnormal changes may appear on X-rays within approximately 1 to 3 months or sometimes even later. Dentists indicate that once the pulp and infection are treated, the tooth begins the healing process. However, if a patient notices failed root canal symptoms—such as persistent pain, swelling, or a returning abscess—the structure of the jawbone may not show immediate filling of the treated root area. In such cases, the empty space remains visible on the X-ray, requiring further clinical assessment to ensure the infection has not returned.
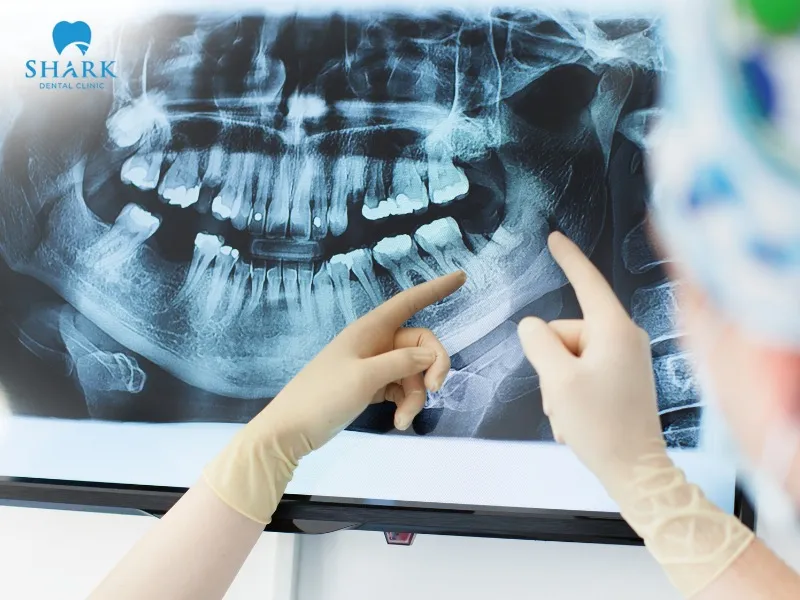
Here’s an overview of the recovery process for the damaged area after root canal treatment and infection management:
- During the first few weeks: In the initial weeks following a root canal treatment, you may not notice any significant changes on X-rays compared to before the treatment. Areas of bone resorption will remain the same size, and the dark shades on the film will not yet show improvement.
- After 6–12 months: The 6 to 12-month period is crucial for evaluating treatment results following a root canal. By this time, many patients begin to show signs of recovery: dark areas around the root tips tend to decrease, and the bone margins visible on the X-ray become clearer.
- After 1–4 years: The healing process following root canal treatment and a dental abscess may continue for several years or longer, particularly if the infection was extensive. If recovery is progressing well, X-rays will reveal clear bone margins without any dark oval or circular areas.
In summary, changes on X-rays after root canal treatment can vary, and the timing of healing depends on the extent of the infection and the individual’s condition. By evaluating the visual progress of a dead tooth root canal before and after the procedure, a dentist can verify that the bone is successfully regenerating and the infection has fully cleared. It’s always advisable to maintain regular dental check-ups to monitor recovery progress following a root canal!
>>> See more: What does cancer look like on dental X-ray?
Will a dentist do a root canal if there is an abscess?
When the pulp of a tooth develops an abscess, a dentist can proceed with root canal treatment. The goal of this treatment is to completely remove dead pulp tissue, eliminate bacteria inside the pulp chamber, and address the abscess to prevent the infection from spreading.
Depending on the severity of the abscess and the condition of the tooth, dentists may take different approaches:
- Localized abscess: In cases of a localized abscess, the dentist will open the pulp chamber and thoroughly clean the root canal. This process helps drain some of the inflammatory fluid and relieves pressure on the tooth. In some instances, a medicated dressing may be placed inside the canal to reduce inflammation and kill bacteria.
- Swollen abscess: If the abscess is significantly swollen and accompanied by severe pain, fever, and fatigue, surgical drainage may be required. This involves making an incision in the abscess, widening the root canal, and removing the affected pulp. After this procedure, the dentist may prescribe painkillers, anti-inflammatory medications, and antibiotics if there are signs of a spreading infection.
- Broken root canal tooth: If the abscess is severe and the tooth is extensively damaged—such as a broken root canal tooth with fractured roots or an irreparable structure—extraction may be necessary. Removing the tooth helps eliminate the infection completely and prevents it from spreading further.
- Use of antibiotics: In many cases, a professional may prescribe specific medications, such as amoxicillin after root canal therapy or abscess drainage, to manage the infection. These antibiotics help reduce symptoms of systemic infection, such as fever, widespread swelling, or difficulty breathing, ensuring the bacteria do not spread further into the jaw or bloodstream.
- Tooth replacement options: After an extraction, dentists often recommend considering dental prosthetics, implants, or bridges. These solutions help restore aesthetics, chewing function, and overall oral health.
Additionally, the dentist will provide detailed guidance on oral hygiene, at-home care, and dietary recommendations. Following these instructions is essential for maintaining a healthy and confident smile.
Taking an abscessed tooth infected root canal X-ray is often necessary to evaluate the extent of damage, inflammation, and abscess development. We hope the information provided here enhances your understanding of root canal X-rays and helps you maintain good dental care.
>>> See more: What is the best antibiotic for root canal infection?